Simulation Educator...or High Reliability Partner?
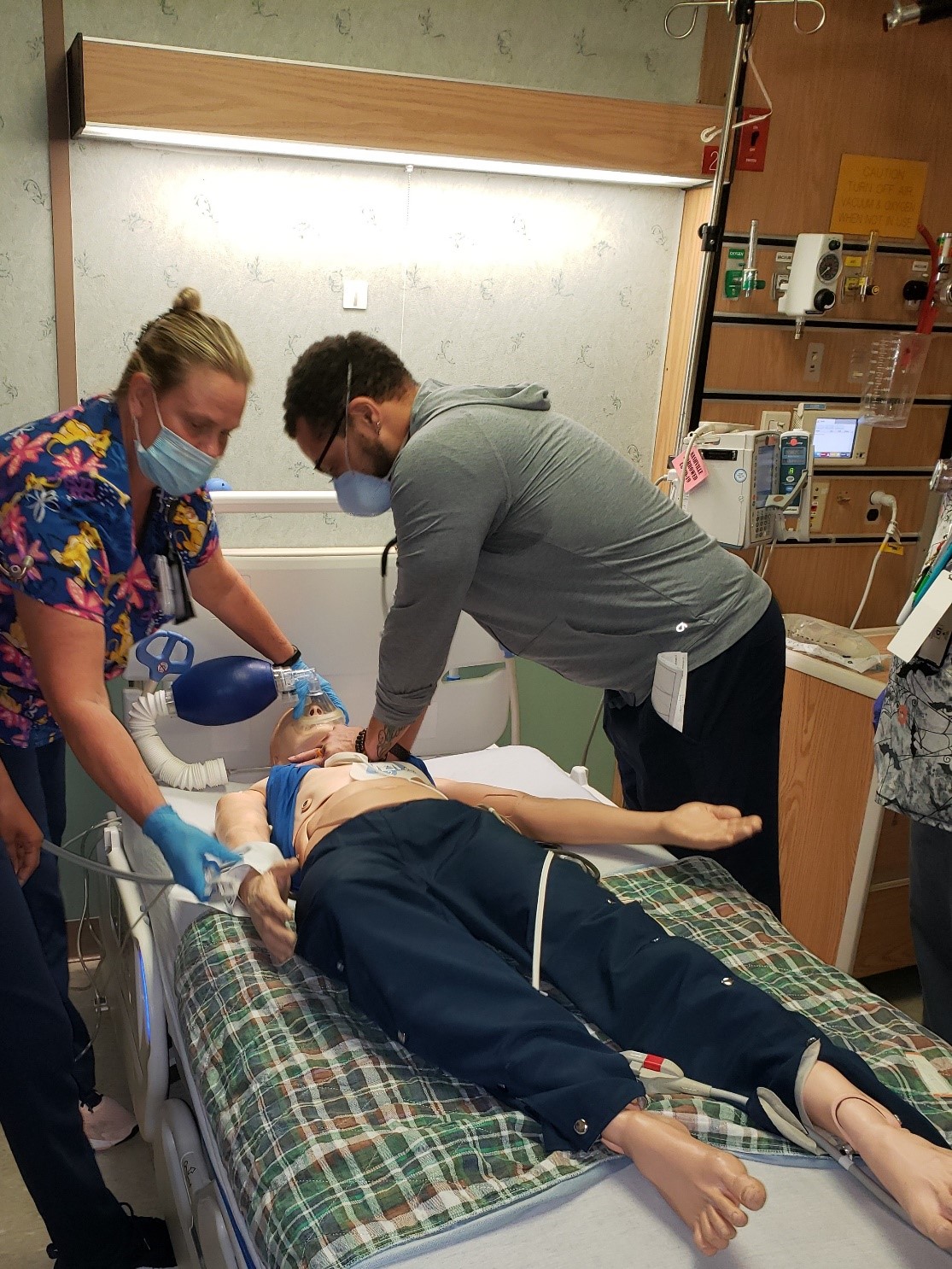
Photo: Beth Davis RN (left) and Dr. Anderson (right) work together during an interprofessional emergency event simulation. Interprofessional team in-situ simulation helps professionals to identify issues which may impact outcomes for Veterans. Photo courtesy of Shelley Lee.
By: Shelley Lee, DNP, RN,C-NIC, CMSRN, CPHRM, CPSO, BC-NPD, Clinical Nurse Educator, Tennessee Valley Healthcare System, Nashville, TN
How do you see your role as a Simulation Educator? Do you characterize yourself as a staff development specialist, an educator, a competency assessor or do you see yourself as an integral member of an interprofessional Quality, Safety, Risk team? Take a moment to consider how your work impacts the patient. You are indeed a key member of the patient safety and quality team who helps to ensure that VA structures and processes result in the patient outcomes that our Veterans deserve.
The simulations you provide for staff support enhanced learning and competence. Perhaps you haven’t considered how those simulations might also provide additional opportunities to impact the operations, processes, and patient outcomes at the VA. In situ simulation, which moves simulation out of the laboratory setting and into the actual workspace, furthering the goal of becoming a High Reliability Organization through the identification of potential failures in both systems and processes.
By conducting simulation within the everyday work environment, fidelity is maintained in a manner that cannot be mimicked in the lab. In situ simulations embrace the messy chaos of healthcare and impose real world concerns without directly compromising patient safety or outcomes (Paige, et al., 2018). Within this messy reality, the failures of an idealized care process or procedure collides with reality uncovering issues previously unknown allowing for risk mitigation.
Recent in situ simulation exercises at Tennessee Valley Healthcare System have identified opportunities to improve quality, safety, and performance. Some of the gaps discovered were a failure to install overhead speakers in a patient care area; inadequate door access; staffing patterns no longer supporting assigned responsibilities; and the opportunity to devise a checklist to prevent errors of human fallibility. These simulations have provided staff with opportunities to identify systems failures impacting their daily work through engagement and empowerment as experts in their workplace. This deference to staff expertise, and the building of resiliency helps to reenforce the principles of high reliability. So, my fellow Simulation Educators, embrace your new role…High Reliability Partner. Carpe diem!!!
Reference:
Paige, J., Fairbanks, R., & Gaba, D. (2018). Priorities related to improving healthcare safety through simulation. Society for Simulation in Healthcare, 13(8), S41-50.



















